Stroke. CVA. TIA. These words mean a death sentence for 150,000 people every year in the UK and leave another 300,000 chronically disabled. Stroke is the third biggest killer of humans worldwide, and dog-owners need to know about it because dogs suffer from strokes too.
In fact, stroke in dogs is much more common than we thought it was a few years ago.

This is what this article is about –
- What you need to know about stroke.
- How it affects dogs.
- Why the weather is important.
- How you can know if your own dogs are at risk and…
- …if so, what you can do to try and avoid it ever happening to them.
So, this is an important article for all dog lovers, please share it widely with everyone you know.
To give you the big picture, we start with a brief summary of what stroke is in humans, then move on and concentrate on stroke in dogs, including the similarities and differences to stroke in humans.
The human perspective
First, the good news
The average life expectancy in humans has dramatically increased over recent decades. From 1950 to 2000, the number of people aged over 60 has increased by 300%, and by 2050 it is predicted to more than triple again. Of course, there are many factors responsible for this including, increased wealth, better education, better nutrition and better public health awareness and advances in medicine.

Despite our increased longevity, the annual worldwide death rate as a result of largely preventable, chronic diseases remains stubbornly high at 36 million. Furthermore, these diseases lead to long-term disability, which is an expensive and unnecessary extra burden for the health services. Lifestyle-related diseases include stroke, heart disease, respiratory disease, diabetes, cancer and obesity. These diseases are associated with behaviours such as smoking (more about smoking HERE), unhealthy diet choices, physical inactivity and high blood pressure.
And there’s more bad news
As a result of the aging population, by 2020, deaths from stroke will have increased by an estimated 200%. In the UK, after heart disease and cancer, stroke is the third largest killer responsible for around 150,000 deaths a year. Having a stroke is not always fatal, but it has led to long-term moderate to severe disabilities in about 300,000 in the UK. The total annual cost of stroke to the UK economy is around £11 billion.
Not surprisingly, therefore, in wealthier countries, prevention of these chronic diseases in as many people as possible has been a long-term goal for governments for decades. The most common risk factors are targeted are high blood pressure, salt intake, more exercise, healthier diet, obesity and tobacco smoking.
About 1 billion people worldwide have high blood pressure and it is solely responsible for about 65% of all strokes. Of those strokes that are fatal, for every 10 deaths, 4 could have been prevented if blood pressure had been managed properly.
For example, it is well known that high salt consumption contributes to high blood pressure, yet manufacturers of processed foods continue to add extra salt (NaCl) to their products to increase palatability and shelf life. This, along with the salt many of us habitually shovel over every meal ourselves, means that most of us consume well over our actual daily need of less than 1g per day.
Alarmingly, the worldwide average salt intake per person per day is between 5g and 18g!
The canine perspective
With over 400 different breeds, varying in size from the tiny-small to the super-large, dogs are unique and really unusual in the animal kingdom. Furthermore, they are one of the few non-human animals to routinely enjoy living out the full length of their lifespan.

Overall, after allowing for body weight, gender and neuter status, cross-breed dogs outlive their pure-breed counterparts by 1.2 years. This age advantage of cross-breeds is most likely due to genetics, i.e. hybrid vigour.
The most common causes of death is UK dogs less than 3 years old are behavioural problems, gastro-intestinal disease and trauma. In contrast, the most common causes of death in dogs older than 3 years are neoplasia (cancer), musculoskeletal disease and neurological disease (which would include stroke). Although ‘old age’ has been quoted as the second most common cause of death after neoplasia, the term ‘old age’ is meaningless unless specifically confirmed by post-mortem examination that can rule out all potentially fatal underlying diseases.
The mechanics of stroke
Stroke is the general term used when the blood supply to the brain is suddenly interrupted and the most common causes are thrombosis, embolism and haemorrhage.
Thrombosis: A thrombosis is caused when the blood starts to clot at a point of ‘roughness’, or damage on the inner wall of a blood vessel. This acts as a seed for further clotting and the clot continues to grow until it eventually obstructs the blood vessel. Alternatively, a clot can break off and get carried away in the circulation, where it becomes an embolism.
Embolism: An embolism is caused when a piece of solid debris floating freely around in the circulation gets lodged as it passed through a narrow blood vessel and blocks it. The most common embolisms are made of blood (thrombus), fat (fat embolism), or air (air embolism).
Haemorrhage: A haemorrhage is the escape of blood from the circulation into the surrounding tissue, where the swelling it causes can obstruct the blood flow to the surrounding tissues.
The anatomy of the brain and its blood supply is very similar in humans and dogs. In addition, like humans, pet dogs live out their natural lifespan and, as a result, are more likely to diseases such as obesity, heart disease and diabetes. Many pet dogs are also exposed to environmental toxins such as pollution and cigarette smoke. It’s hardly surprising then that dogs, like humans, suffer from strokes.
So, stroke is a disease of the blood supply to the brain, the cerebrovascular system, accounting for its medical name, a cerebrovascular accident (CVA). However, this term is reserved for stokes where the clinical signs last more than 24 hours. If the clinical signs of the stroke disappear in less than 24 hours, this is a transient ischaemic attack (TIA).
Ischaemia is a reduction in the blood supply leading to the starvation of oxygen and glucose to the tissues being supplied. Brain cells are very greedy and they quickly deteriorate and die if starved of blood for any length of time. When an area of tissue dies as a result of ischaemia, it is called an infarction. So, a TIA and a CVA are essentially the same thing, but differ in duration. The location of the stroke in the brain is also important – a TIA in one area may manifest itself as a CVA, had it occurred in a more functionally critical area of the brain (remember, the presence or absence of clinical signs determine the name).
A stroke is also classified according to what caused it. An ischaemic stroke is caused by a thrombosis, or an embolism, while a haemorrhagic stroke is causes by a haemorrhage.
In humans, 77% of all strokes are ischaemic, while 23% are haemorrhagic. Atherosclerosis (a build-up of fatty deposits in the blood vessels) is a common cause of ischaemic stroke by embolism. Having high blood pressure is the biggest risk factor for stroke in humans and one of the reasons for this is that it promotes the development of atherosclerosis.
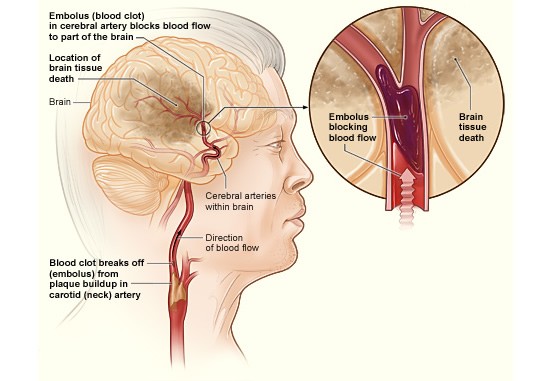
Image by National Heart Lung and Blood Institute (NIH) [Public domain]
Stroke in dogs
By comparison, haemorrhagic strokes are rare in dogs. However, in dogs with chronic diseases such as hypothyroidism, diabetes mellitus, hyperadrenocorticism and hereditary hypercholesterolaemia, ischaemic stroke by embolism as a result of atherosclerosis is more common. Unlike humans, high blood pressure on its own is not common, but it can occur in dogs with chronic diseases such as renal disease and hyperadrenocorticism, thereby increasing the risk of stroke.
Overall, while stroke is a common neurological disease in humans, and it is the third biggest killer, this is not the case in dogs where it is relatively quite rare, accounting for around 1.5 to 2% of all neurological cases seen.

The brain’s blood supply is the critical factor
As mentioned above, the brain is a very greedy organ and it needs a constant and reliable blood supply to all parts. Every cell must have oxygen, glucose and other nutrients, and just as important, the efficient removal of waste products, such as carbon dioxide and lactic acid. To achieve this, the brain has 5 pairs of main arteries. The rostral, middle and the caudal cerebral arteries together supply the cerebral cortices and surrounding areas at the front of the brain. The rostral and caudal cerebellar arteries supply the cerebellum and surrounding areas at the back of the brain.
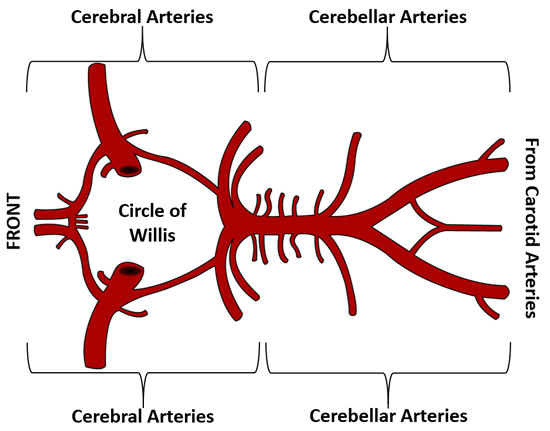
Image by [Public domain], adapted and labelled by RFT
Yet, despite this elaborate blood supply, accidents still happen. In humans, it takes a reduction in blood flow of less than 40% of normal for ischaemia to start to occur in the brain. This is probably the same for dogs.
The clinical signs of stroke
The most obvious clinical sign of an embolic stroke is the speed at which it becomes apparent, like turning off a switch. For a thrombotic or a haemorrhagic stroke, the onset of clinical signs can be immediate, but they can also be slightly delayed.
Like in humans, how an individual dog is affected by the sudden-onset of neurological deficits depends entirely on where the stroke is in the brain and how widespread it is. Typically, the clinical signs that are observed can give a clue as to where in the brain the problem occurred (but there are always exceptions to this of course), for example –
Forebrain: A weakness down the left or right side of the body. Difficulty in leg-hopping on the affected side of the body when the opposite leg is lifted. Walking in circles. Seizures in some dogs. Note that the affected side of the body, left or right, will be the opposite side to that where the stroke occurred.
Cerebellum: Movement of the limbs may be jerky, clumsy and exaggerated. Vestibular signs indicate that the vestibular system, that controls balance and orientation, has been affected. Signs include difficulty in maintaining balance, as if drunk. Constant, rapid, uncontrolled eye movements (nystagmus). A squint in one eye, that is, both eyes not simultaneously looking in the same direction (strabismus). Circling. Head tilt. Arching of the head and neck backwards (opisthotonus). Note that the affected side of the body, left or right and most obvious in head tilt and circling, will be the same side to that where the stroke occurred.
Brainstem: 10 of the 12 cranial nerves originate in the brain stem so the signs of stroke can be similar to those described for the cerebellum above. A weakness down one or both sides of the body. Circling. Head tilt, or turning. Note that the affected side of the body, left or right and most obvious in head tilt and circling, will be the same side to that where the stroke occurred.
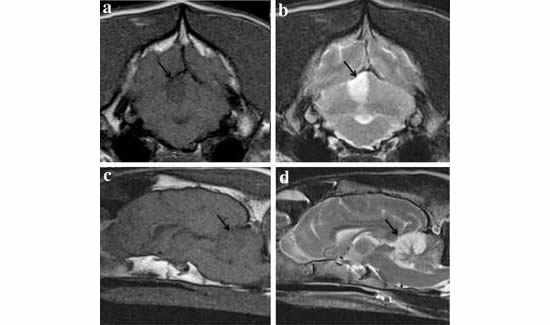
Image by Thomsen et al. (2016). doi.org/10.1186/s13028-016-0219-2 is licensed under CC BY 4.0 (http://bit.ly/1rMF155)
Stroke in dogs, the veterinary perspective
There is no specific treatment for stroke in dogs beyond supporting any of the neurological deficits if required, for example seizures.
In humans, the mortality rate for ischaemic stroke is between 10% and 17% 30 days after the stroke and between 15% and 29% a year later. Other factors that increase mortality rate in humans are the presence of other chronic diseases such as heart disease, age and having another stroke. 15% to 20% of humans have another stroke within 5 years and mortality rate is higher in this group.
The prognosis for most dogs after a stroke is generally good and most recover within a few weeks. However, this does depend on the severity of the stroke as indicated by the clinical signs. It also depends on the dog’s overall health prior to the stroke. In dogs with concurrent diseases such as renal disease, hypothyroidism, diabetes mellitus, hyperadrenocorticism and hereditary hypercholesterolaemia, the long-term prognosis can be less favourable. Although much less common in dogs, haemorrhagic stroke is associated with a higher mortality rate than ischaemic stroke.
There is a huge pool of data on stroke in humans going back many decades from which information about long-term outcomes has been collated. This is not the case in dogs, but there is 1 study that has analysed the clinical data for 22 dogs over four and a half years following an ischaemic stroke. In this study MRI diagnostic imaging was used to identify the exact location of the stroke and its extent within the brain, which was then compared with what was actually observed clinically.
In this study, there were 15 males and 7 females, ranging in age from 2 to 17 years old. The stroke in each dog manifested as the sudden onset of one or more of the following clinical signs (the number in brackets reflects the number of dogs) – seizures (13), a weakness down one or both sides of the body (13), difficulty in maintaining balance, as if drunk (7), mental changes (6), deficits in vision (3).
The MRI scans showed that the stroke was in the forebrain in 19 dogs and in the cerebellum in 3 dogs. The locations and prevalence of these strokes were similar to those found in humans. In 13 dogs, the stroke was on the left side of the brain, while in the other 9 it was on the right.
4 of these dogs had other, ongoing medical conditions. 3 had heart disease, 1 had a small tumour and 1 had hyperadrenocorticism (Addison’s disease). However, this information was excluded from the overall data analysis because the total number of dogs in the study was just too small to make it useful.
Of the 22 dogs included in this study, 5 dogs were euthanased at the owners request within 30 days of their strokes because they all suffered additional strokes. For the remaining 17 dogs, the median survival time was 505 days (about 16 months). 7 of these dogs had a second severe stroke 6 to 17 months after the first stroke, and they either died or were euthanased on humane grounds. 3 of these dogs died of unknown causes 7, 19 and 32 months after their stokes. For the remaining 7 of the 17 dogs, the long-term outcome was considered excellent, as judged by their owners. In other words, these dogs continued to have a good quality of life after their strokes. The only long-term problem reported for 2 of the dogs was a behavioural change described by their owners as a subtle ‘loss in confidence’. Furthermore, 4 of these dogs were still alive four and a half years after their strokes when the study ended.
TAKE-HOME MESSAGE
From the veterinary perspective, the message here is that, if they survive the early stages beyond 30 days, the prognosis for dogs that suffer a stroke is fair to good. Statistically, in this study, 17 of the dogs (77%) survived the first 30 days and all of them went home and continued to enjoy life for some considerable time. It was only later on that, for 10 of these dogs, the prognosis was changed for the worse.
The pattern of recovery following stroke reported by the owners of these dogs was similar to that reported in humans. Over the first 2 to 4 weeks, recovery was quickest and then became more subtle and less obvious week-to-week for the next 12 months following the stroke. The loss of confidence in 2 of the dogs, as reported by 2 of the owners, is a well-known phenomenon in humans.
In humans, about 9% of stroke victims suffer with seizures as one of the clinical signs and this increases the risk of mortality both before 30 days and up to a year post-stroke. In this study, 13 of the 22 dogs (59%) had seizures, but it did not have the same negative effect on survival time.
Of the risk factors looked at in this study (age, gender, body weight and side of the stroke, left or right), only 1 significant predictor of prognosis was identified, the side of the brain that the stroke occurred. Strokes on the left side of the brain increased the chances of survival after 30 days 16-fold compared to strokes on the right. The mean survival time for a left-sided stroke was 602 days, compared to just 24 days for right-sided strokes.
Stroke in dogs, the effect of the weather
As discussed above, there are many factors, or triggers, that increase the risk of having a stroke in both humans and dogs. For example increasing age, high blood pressure, high cholesterol, hyperlipidaemia, obesity, diabetes mellitus, hyperadrenocorticism, hypothyroidism, heart disease and kidney disease. All these risk factors are intrinsic and they are predictable. That is, the person, or dog either has them, or they do not. And, as such, all of them can be controlled to some degree using medication in combination with lifestyle changes.
But, what about extrinsic risk factors that are beyond the influence of control using drugs, etc.? For example, environmental factors like the weather. Changes in weather lead to transient (and sometimes unpredictable) changes in ambient temperature, atmospheric pressure and humidity. Although the link between a change in the weather and having a stroke may sound like unfounded superstition, it’s not as crazy at it seems if you think about the physiology.
Every winter, a drop in ambient temperature triggers the body’s cold reflex which activates the sympathetic nervous system (SNS). The SNS causes small blood vessels in the extremities to constrict which reduces the blood flow, thereby conserving body heat, but it also increases blood pressure. In addition, the stress hormones themselves (adrenaline and noradrenaline) released by the SNS also increase blood pressure independently. Cold temperatures also increase blood cholesterol, fats and blood clotting factors.
It comes as no surprise, therefore, that more people have strokes – and die from strokes – during the autumn to winter transition. But it’s not just falling temperatures. In humans, the current data suggests that small fluctuations in temperature – up or down – increase the risk of having a stroke. The greatest risk factor is a rapid change in weather conditions.
Could the weather also increase the risk of stroke in dogs? The answer to this question is that we don’t know, or at least we didn’t. But we do know now because someone has studied the phenomenon.
In this weather study, the medical records of 15 dogs (10 males and 5 females) that had suffered a stroke, confirmed by MRI scan, were obtained. In addition, the local meteorological data on temperature, pressure and humidity was also obtained for the 8 days preceding the dates that the dogs had their strokes. Although the number of dogs involved in this study is small, it is really interesting because the data was collected over a 5-year period (2011 to 2015) and so reflects both annual and seasonal variations in weather conditions. For example mean daily temperatures over the 5 years varied from a low of -9.31°C to a high of +22.08°C.
As suspected, most of these dogs had their strokes as the ambient temperatures were changing through autumn to winter period September, October and November.

Image by Meadows and Silver (2017). doi:10.3390/vetsci4040056 is licensed under CC BY 4.0 (http://bit.ly/1rMF155)
Drilling down into the data in more detail yields more…
AMBIENT TEMPERATURE
** 5 of the strokes corresponded with a significant decrease in ambient temperature.
** 2 of the strokes corresponded with a significant increase in ambient temperature.
** 8 of the strokes did not correspond to a significant change in ambient temperature.
What does this mean? It means that 7 of the 15 strokes (47%) corresponded with a rapid change in ambient temperature (up or down) of 4.5°C.
APPARENT TEMPERATURE
The apparent temperature is another way of measuring ambient temperature by taking into account the prevailing wind speeds and humidity. It is commonly used by weather forecasters (look at the online UK BBC, or Met Office forecasts for good examples) because it more accurately reflects how cold it actually feels. For example, on a day where the ambient temperature is -1°C, if there is also a cold wind blowing, the apparent temperature could be shown on the weather forecast as -6°C. This is commonly called wind chill.
** 7 of the strokes corresponded with a significant decrease in apparent temperature.
** 3 of the strokes corresponded with a significant increase in apparent temperature.
** 5 of the strokes did not correspond to a significant change in apparent temperature.
What does this mean? It means that 10 of the 15 strokes (67%) corresponded with a rapid change in apparent temperature (up or down) of 4°C.
PRESSURE
** 6 of the strokes corresponded with a significant decrease in pressure.
** 6 of the strokes corresponded with a significant increase in pressure.
** 3 of the strokes did not correspond to a significant change in pressure.
What does this mean? It means that 12 of the 15 strokes (80%) corresponded with a rapid change in pressure (up or down) of 6.8 mmHg.
HUMIDITY
** 7 of the strokes corresponded with a significant decrease in humidity.
** 4 of the strokes corresponded with a significant increase in humidity.
** 4 of the strokes did not correspond to a significant change in humidity.
What does this mean? It means that 11 of the 15 strokes (73%) corresponded with a rapid change in humidity (up or down) of 15%.
TAKE-HOME MESSAGE
In this weather study, many of these dogs had their strokes during periods of change in the weather characterised by rapid fluctuations – up or down – in temperature, pressure and humidity. The important trigger factor here is change. To put some numbers on this, changes – up or down – in temperature of 4.5°C, or pressure of 6.8 mmHg, or humidity of 5%. These figures correspond with those found in studies of human stroke environmental triggers.
As stated above, the number of dogs involved in this study were small (human studies routinely involve between 200 to more than 2 million people), but the fact that the results agree with those from human studies does suggest that it is reasonable to conclude that the data presented here is a useful addition to our current knowledgebase on stroke in dogs.
© copyright Robert Falconer-Taylor, 2018
This article is an original work and is subject to copyright. You may create a link to this article on another website or in a document back to this web page. You may not copy this article in whole or in part onto another web page or document without permission of the author. Email enquiries to robertft@emotions-r-us.com.
References
Brinsden, H.C. and Farrand, C.E., 2012. Reducing salt; preventing stroke. Nutrition Bulletin, 37(1), pp.57-63.
Gredal, H., Toft, N., Westrup, U., Motta, L., Gideon, P., Arlien-Søborg, P., Skerritt, G.C. and Berendt, M., 2013a. Survival and clinical outcome of dogs with ischaemic stroke. The Veterinary Journal, 196(3), pp.408-413.
Gredal, H., Skerritt, G.C., Gideon, P., Arlien‐Soeborg, P. and Berendt, M., 2013b. Spontaneous ischaemic stroke in dogs: clinical topographic similarities to humans. Acta Neurologica Scandinavica, 128(3).
Meadows, K.L. and Silver, G.M., 2017. The Effects of Various Weather Conditions as a Potential Ischemic Stroke Trigger in Dogs. Veterinary sciences, 4(4), p.56.
O’Neill, D.G., Church, D.B., McGreevy, P.D., Thomson, P.C. and Brodbelt, D.C., 2013. Longevity and mortality of owned dogs in England. The Veterinary Journal, 198(3), pp.638-643.
PDSA, 2017. PDSA Animal Wellbeing Report (PAW) 2017. http://bit.ly/2ErrFmV. Accessed 02/01/2018.
Thomsen, B., Garosi, L., Skerritt, G., Rusbridge, C., Sparrow, T., Berendt, M. and Gredal, H., 2016. Neurological signs in 23 dogs with suspected rostral cerebellar ischaemic stroke. Acta Veterinaria Scandinavica, 58(1), p.40.
Thomsen, B.B., Gredal, H., Wirenfeldt, M., Kristensen, B.W., Clausen, B.H., Larsen, A.E., Finsen, B., Berendt, M. and Lambertsen, K.L., 2017. Spontaneous ischaemic stroke lesions in a dog brain: neuropathological characterisation and comparison to human ischaemic stroke. Acta Veterinaria Scandinavica, 59(1), p.7.
Wessmann, A., Chandler, K. and Garosi, L., 2009. Ischaemic and haemorrhagic stroke in the dog. The Veterinary Journal, 180(3), pp.290-303.